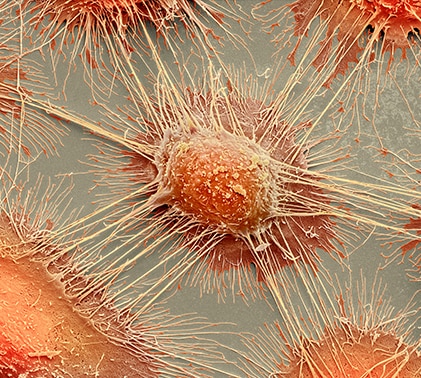
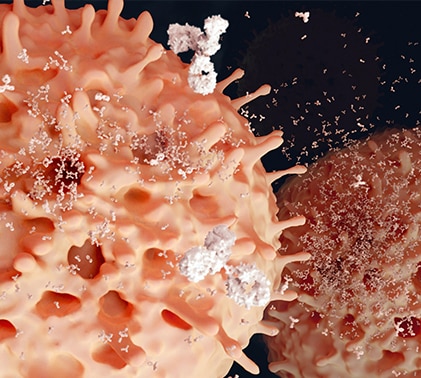
IMMUNO-ONCOLOGY IS ON THE CUSP OF A SURGE FORWARD
"I had a desire to do something meaningful." This was biologist Laura Helming’s answer when asked about her decision to dedicate herself to the field of immuno-oncology. Her path toward this branch of medicine, which uses the body's own immune system to fight cancer cells, involved a series of intermediate stages. When Helming studied biology as a student, she was particularly interested in genetics and infectious diseases. As the immune system and infectious diseases are inherently linked, the decision to pursue immunology was a logical next step.
After working in the area for several years, Helming was given the chance in 2013 to work for Merck KGaA, Darmstadt, Germany in the field of immuno-oncology. She refers to working at the intersection of immunology and oncology and exploring new therapies fight cancer as an “incredible opportunity.”
“It's a privilege to be able to work as a scientist in this field,” says Helming.